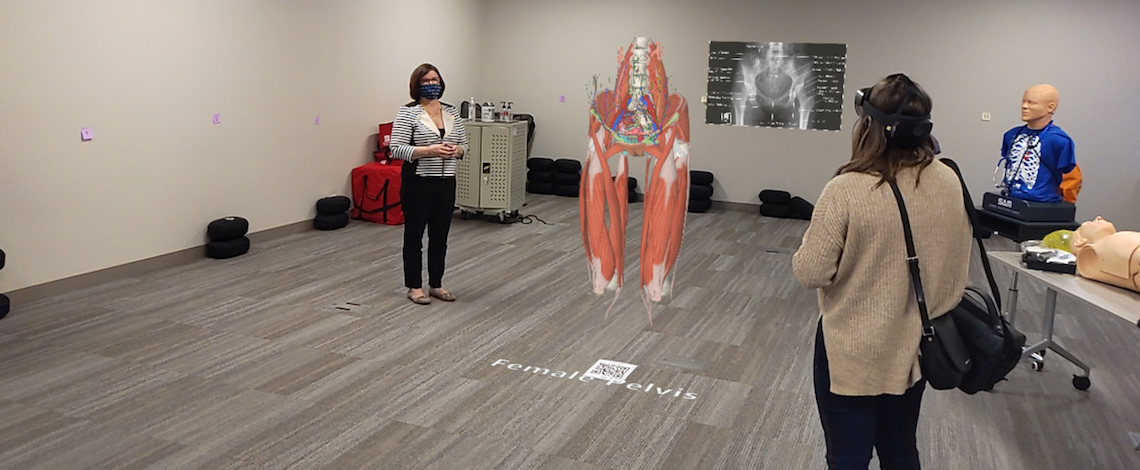
Leslie Catron showcases holoanatomy, which can only be seen virtually using HoloLens technology.
Written by Breanna Hardy
The health care industry is setting its sights on virtual reality as the next frontier for technological advancement.
California Health Sciences University in Clovis operates its simulation center with immersive technology. One of the latest pieces of technology, the Butterfly Probe, is a handheld, bedside ultrasound system expected to allow for an increase in-home care or care in rural areas with lack of health care access.
The hand-held device will hook up to an app on a smartphone, allowing doctors to monitor a fetus anywhere — on the spot in the emergency room or for at-home care purposes. This is much more efficient than waiting for an ultrasound technician to come and bring all the equipment in a room, said Simulation Center Director Leslie Catron.
Students receive a Butterfly Probe with their tuition costs.
“The statement is it’s going to take the place of the stethoscope in the future because you can see the heartbeat, you can see how fast the heart’s going, you can see the blood flow in the heart, you can see the abdomen. You can see joints and bones,” Catron said.
There are other opportunities for mobile health care, too. Get Well, a digital health company, is partnering with Adventist Health. Hanford will see Get Well integrated into its patient care model.
The app gives patients access to resources during their hospital stay via their mobile device. It also helps alleviate staff shortages. Patients can order meals, communicate with doctors, view their medications and complete their discharge checklist via Get Well. The digital platform allows for patients to handle administrative or non-clinical tasks, allowing nurses to focus on patient care.
At CHSU, immersive technology is training students for cutting-edge advancements in health care.
Ralph Herrera, simulation operations specialist, helps facilitate CHSU’s use of the Microsoft HoloLens, a pair of mixed reality glasses that allow students to study material via holograms.
“The benefit of having HoloLens and holoanatomy is that you can study wherever you are, whether that’s at home, or at your friend’s house, or even at Starbucks. As long as you have WiFi, it’ll connect and it’ll link to the cloud,” said Luis Felipe Vargas-Marquina, anatomy technology facilitator.
Catron said that this technology made pivoting to online learning early on in the pandemic much more seamless. And while students prefer to learn together in person, the components of the class didn’t change even while on Zoom.
“The actual HoloLens itself is just a computer on your face, and it has apps that you can add to it,” Catron said.
Catron said that hospitals are warming up to the idea of adopting this kind of technology. With the mixed reality glasses, doctors can consult with one another remotely if needed.
“That’s only just beginning. There’s crazy things that are going to happen with that,” she said.
Catron said that Herrera was instrumental in creating the online setup for the students to use HoloLens in their homes when the school was 100% virtual.
Students were placed in different scenarios with patients via Zoom, where they could interact with patients virtually. Catron said it was a form of telemedicine.
“That is really what came out of Covid — telemedicine just went and skyrocketed,” she said.
“We were able to present or display the patients’ X-rays. We also were able to project labs, relay the lung sounds and the heart sounds,” Herrera added.
Since that time, CHSU has been granted provisional accreditation from the Society for Simulation in Healthcare. CHSU’s Simulation Center will be eligible to apply for full accreditation in 2023.
The Society for Simulation in Healthcare is the largest health care simulation accrediting body in the world, with over 100 accredited programs in 10 countries.
They examine a simulation program’s processes and outcomes in core provisional and companion requirements in assessment, research, education and systems integration.
CHSU also uses high-fidelity manikins to study anatomy. The manikins are common in the nursing world and are relatively new in the medicine world, which has stuck traditionally to live people.
“Research shows that using interactive simulation experiences combined with classroom learning develops better-prepared clinical practitioners while improving quality health care, education and patient safety,” said Catron.
Hospitals haven’t typically offered manikins to practice and train on, and while it’s seeing improvement, Catron said it’s up for debate for a couple reasons.
It’s expensive to operate these high-fidelity manikins, and many hospitals struggle with the ethical debate of spending money on real patients or spending money on the manikins that allow for strategic training. It also requires that hospital staff employ someone who knows how to operate the manikins.
“Putting in technology that is for training and education, even though it touches a person eventually, is one of those balancing acts when you’re sitting in front of the board,” Catron said.
When looking at the advancements of health care, Herrera says that virtual reality is the big thing.
“We’re starting to see virtual surgical procedures,” he said.








